Updates from the ACR Convergence 2023 Review Course, part 1
Updates from the ACR Convergence 2023 Review Course, part 1
SAN DIEGO—The pre-conference Review Course at ACR Convergence 2023, moderated by Noelle Rolle, MBBS, assistant professor in the Division of Rheumatology, associate program director of the Rheumatology Fellowship at the Medical College of Georgia, Augusta University, and Julia Schwartzmann-Morris, MD, associate professor, Donald and Barbara Zucker School of Medicine at Hofstra/Northwell, Great Neck, N.Y., tackled numerous important topics in rheumatology. Here, we report on the first presentation of Saturday, Nov. 11.
Laura Kopplin, MD, PhD, assistant professor of ophthalmology and visual sciences, University of Wisconsin, Madison, discussed inflammatory disease of the eye. Dr. Kopplin began her talk by describing key concepts in uveitis.
Uveitis
Many rheumatologists see patients referred for uveitis, and Dr. Kopplin noted that it is essential the specific type of uveitis (i.e., anterior, intermediate, posterior or panuveitis) be identified because the differential diagnosis for each condition is different.

Dr. Laura Kopplin
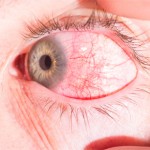
Anterior uveitis is the classic form—the one many clinicians think about when they hear uveitis. Anterior uveitis is defined by the presence of cells or cellular aggregates visible in the anterior chamber of the eye on exam. This tends to be painful for most patients, although it may be asymptomatic in patients with juvenile idiopathic arthritis (JIA).
Common causes of anterior uveitis include spondyloarthropathies, sarcoidosis, Behçet’s disease and a number of infections, such as syphilis and tuberculosis. Dr. Kopplin provided several clinical pearls, including:
- Inflammatory bowel disease-associated anterior uveitis tends to be bilateral; and
- Tubulointerstitial nephritis and uveitis (TINU) syndrome may be an under-recognized cause of anterior uveitis.
TINU is more common in younger patients, may present with bilateral anterior uveitis and diagnosis may, in part, rely on testing urine beta-2 microglobulin, which is elevated in the condition.
Regarding prognosis, the Standardization of Uveitis Nomenclature (SUN) Working Group is an international group of experts that has created a grading system for anterior uveitis, which can help predict the risk of vision loss in patients.
Intermediate uveitis is a form of the condition that mostly manifests with vitritis. To diagnose the condition properly, a dilated eye exam is needed. There is an association between multiple sclerosis (MS) and intermediate uveitis, but Dr. Kopplin does not recommend obtaining magnetic resonance imaging (MRI) studies of the brain and spinal cord routinely in all patients with intermediate uveitis. Rather, such testing should be based on risk factors for, or signs of possible, MS. Intermediate uveitis can be graded using the degree of vitreous haze, which is based on the clarity of view of the posterior segment on funduscopic exam.