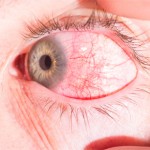
Treatment
Treatment for inflammatory diseases of the eye almost always starts with topical corticosteroid therapy. If patients fail to respond adequately, they may then be treated with systemic corticosteroids or shorter acting injectable steroids.
The next step in patients with an inadequate response would be conventional disease-modifying anti-rheumatic drugs (DMARDs), certain biologics and finally alkylating agents when needed. Some of the medications included in these treatment categories are azathioprine, methotrexate, mycophenolate mofetil, cyclosporine and cyclophosphamide.
Even with these treatments, only about 40–50% of patients will gain control of their disease. If DMARD therapy fails to help patients, tumor necrosis factor-α (TNFα) inhibitor therapy is often the next step, with adalimumab and infliximab having the most robust evidence of efficacy; etanercept is less effective. Tocilizumab has been used to treat uveitis, and it appears to work well for patients with persistent uveitic macular edema. Rituximab may be an option for patients with scleritis or orbital inflammatory conditions.
Jason Liebowitz, MD, is an assistant professor of medicine in the Division of Rheumatology at Columbia University Vagelos College of Physicians and Surgeons, New York.