Rheumatologists in the United States earn $150,000–$250,000 per year, with an overall median salary of $173,000, according to the first-ever 2011 Physicians Compensation Report by Medscape, an Internet provider of medical information for physicians and consumers. Compensation remained steady in 2010, the survey year, compared with 2009.
In comparison to other specialists, rheumatologists are closer to the lower end of the scale for compensation. For example, the highest-earning specialists are orthopedic surgeons and radiologists, with a median compensation of $350,000, followed by anesthesiologists and cardiologists at $325,000. On the lowest end of the scale are pediatricians ($148,000), primary care ($159,000), endocrinologists ($165,150), and then rheumatologists. Just above rheumatologists are HIV/infectious disease specialists ($174,750) and psychiatrists ($175,000).
Location, Location, Location
Interestingly, rheumatologists in the Great Lakes region earn $37,500 more than those in the Northeast, according to survey results. A higher income is seen in all specialties in the North Central area of the U.S. (Iowa, Missouri, Kansas, Nebraska, South Dakota and North Dakota), with an average overall median income of $225,000. Among rheumatologists, however, the median income in the North Central area is $167,185.
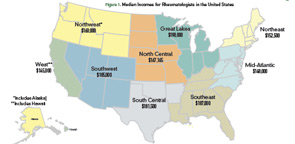
According to the report, median incomes in geographic areas of the country for rheumatologists (see Figure 1) are:
- Northeast $152,500
- Mid-Atlantic $148,000
- Southeast $187,000
- Great Lakes $190,000
- North Central $167,165
- South Central $181,500
- Northwest $160,000
- Southwest $185,000
- West $145,000
Rheumatologists in midsized cities and suburban areas earn almost $20,000 more than their counterparts in major metropolitan areas, Medscape reports.
For More Information
- 2011 Physician Compensation Report: www.medscape.com/features/slideshow/
compensation/2011 - 2011 Rheumatologist Compensation Report: www.medscape.com/features/slideshow/
compensation/2011/rheumatology
Male–Female Pay Gap Persists
In rheumatology, a pay gap exists between male and female rheumatologists, although the gap is narrower than in some other specialties, according to the Medscape analysis. Men earn a median compensation of $180,000 compared with $153,500 for women. Physician recruiters tell Medscape that women are more likely to seek positions that require fewer hours, in order to handle both career and family life.
Across all specialties analyzed, women report a median income of $160,000 compared with $225,000 for men, with the differences especially noted in orthopedic surgery, cardiology, and gastroenterology—the higher-paid specialties.
Additional Findings
Fifty-three percent of the rheumatologists believe they receive a fair wage for their work, but a large salary spread was noted between practice situations. Rheumatologists working in group single-specialty practices earn significantly more than those in solo practices. Beyond compensation, the report found that nearly 40% of rheumatologists spend 30 to 40 hours a week involved in direct patient care, while 23% spend less; only 5% spend more than 50 hours per week. The amount of time spent does not differ between private practitioners and those considered “employees.” More than half the respondents see 50–99 patients a week, 20% see more than 100 patients a week, and 15% see fewer than 25 patients a week.
High rates of satisfaction with medicine as a career (75%) and rheumatology as a profession (66%) are expressed by rheumatologists, but only 49% say they would choose the same practice setting if they could do it over again.
The Medscape survey was conducted from Feb. 2, 2011, to March 30, 2011, with a total of 15,794 responses from all specialties. Of these, 1%, or about 1,500, were rheumatologists.
Rheumatologists Respond What do rheumatologists think about this report?
“The Medscape report is sobering in many aspects, but encouraging in others,” says Abby Abelson, MD, chair of Department of Rheumatology at Cleveland Clinic and chair of the ACR Committee on Training and Workforce Issues. Noting that the report is somewhat limited by a small sample size of responders in rheumatology, she added the placement of rheumatologists at the lower end of the specialties can be “partially explained by the long visit length required in our specialty, which they documented to be over 17 minutes for over 75% of rheumatologists.”
“As we face a large increase in the numbers of patients who will need rheumatologic care in the coming decades, these data may make recruiting new physicians to our specialty challenging,” she adds. “We will need to advocate at all levels for appropriate reimbursement for the great deal of time that is required to appropriately evaluate complex patients with multi-system rheumatic diseases.”
William F. Harvey, MD, assistant professor of medicine in the division of rheumatology at Tufts Medical Center in Boston, says that, “this report is accurate in the sense that rheumatology is ranked near the bottom, but the reality is far worse. First, there are severe regional differences, with the Northeast seeing lower salaries. Second, the median age of the rheumatology workforce is 55 years old. That means that the median salary sited in the article are inflated as >50% of rheumatologists have been in practice for 25 years and thus have higher salaries.”
He adds that changing demographics also impact compensation as “there are more and more part-time rheumatologists; when those 55 or older retire, there will be a huge drop in median salary.” Additionally, the higher debt incurred by recent graduates (median indebtedness $150,000 for the class of 2010 according to a 2010 American Association of Medical Colleges report), plus the expense of additional training and decreased insurance reimbursement compared with other specialties, adds to the financial burden in rheumatology, Dr. Harvey says.
While a positive note is that rheumatologists were happier in their choice of specialty than many other specialties, Dr. Abelson says “this enthusiasm is what we are communicating to our trainees on a daily basis. Our ability to care for patients with challenging and complex conditions over many years, exposure to the most current science with ‘bench to bedside’ impact, and impacting patients’ quality of life and longevity is an honor that accounts for rheumatologists’ high satisfaction rating.”
Dr. Harvey, too, feels that career satisfaction is key for rheumatologists. “Fortunately, the draw to rheumatology has been and will continue to be (unless there is a radical reimbursement reform) love of the field and exposure to our enthusiastic membership who share their love of the field,” he says. “None of us ever chose this for the money, and probably no one ever will.”
Sue Pondrom is a medical journalist based in San Diego.

