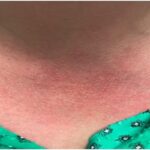
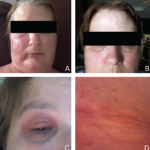
Yao Syndrome (YAOS, OMIM617321)
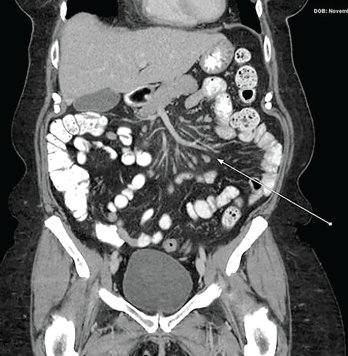
Figure 2: CT of the Abdomen & Pelvis with Contrast
The arrow shows findings of mesenteric panniculitis manifested as increase in density of the mesenteric fat surrounding the mesenteric vessels and increase in size and number of mesenteric lymph nodes.
YAOS, formerly designated as NOD2-associated autoinflammatory disease, is characterized by periodic fever, dermatitis, arthritis and swelling of the distal extremities, as well as GI and sicca-like symptoms.6,20-22 Patients generally have flu-like symptoms, followed by episodic fever and erythematous patches or plaques with pathological finding of spongiotic dermatitis mostly. An episodic flare may last a few days to weeks with an asymptomatic interval of several weeks or months.
GI symptoms are common, including recurrent abdominal pain, cramping, bloating and non-bloody diarrhea, and the symptoms may last several days to weeks. There is no endoscopic, radiological or histopathological evidence of IBD. Oligo- or polyarthritis is common, and occurs periodically without joint erosions, destruction or deformities; joints appear normal when the disease is quiescent. Approximately 25% patients develop intermittent, unilateral or bilateral, distal lower extremity swelling involving the ankles and feet.23 In addition, patients can have oral ulcers and chest pain from pericarditis or/and pleuritis.
The proposed diagnostic criteria for YAOS comprise the characteristic phenotype, specific NOD2 variants and rigorous exclusion of overlapping disease entities.22 The NOD2 variant IVS8+158 is detected in almost all YAOS patients, with concurrent R702W in up to 30%; other, rarer NOD2 variants can be identified in some patients.21
YAOS has been predominantly reported in white adults, with a female to male ratio of 2:1. The mean age of onset is 30 years. The disease occurs sporadically in a majority of patients, and a positive family history is seen in a minority. Although it is a multi-organ disease, YAOS rarely affects solid internal organs.
In addition to the characteristic clinical phenotype, these patients can have episodic asthma/shortness of breath and fibromyalgia/chronic pain syndrome as relatively common comorbidities.22 All in all, the clinical phenotype and genotype in our case indicated YAOS.
Patient’s Course
The therapeutic strategy for YAOS depends on the frequency and severity of the disease flares. Treatment remains empiric and involves intermittent short courses (i.e., several days) of glucocorticoids, sulfasalazine and/or IL-1 inhibitors.22,24 The patient was followed at our rheumatology clinic every six months, during which time she might have one or two mild flares, including fever, rash and abdominal pain. Her flares were managed with short courses of prednisone and symptomatic treatment. Sulfasalazine was not given due to her prior allergy, and the use of any anti-IL-1 biologics was deferred because of more recent mild disease.