Image Credit: ajt/shutterstock.com
Brentuximab Vedotin Enters Phase 2 Trials
Brentuximab vedotin (Adcetris), an antibody-drug conjugate (ADC) directed at CD30, is currently entering Phase 2 clinical trials for treating systemic lupus erythematosus (SLE).1
The ADC encompasses an anti-CD30 monoclonal antibody, which is attached by a protease-cleavable linker to a microtubule-disrupting agent, known as monomethyl auristatin E (MMAE). The ADC was developed to be stable in the bloodstream, but will liberate MMAE when it is internalized into CD30-expressing cells. This Phase 2 trial will help assess the safety and efficacy of brentuximab vedotin in managing adults with SLE. The drug is currently being investigated in at least 30 clinical trials, including four Phase 3 trials for different oncology uses, such as CD30-positive lymphomas.
FDA Reviews Xeljanz Application
The U.S. Food and Drug Administration (FDA) has accepted for review a new drug application for tofacitinib citrate (Xeljanz) 11 mg once-daily modified release tablets to treat moderate to severe rheumatoid arthritis in patients who have had an inadequate response or demonstrated intolerance to methotrexate.2 Preliminary equivalency data have shown comparability between tofacitinib 11 mg once daily and tofacitinib 5 mg twice daily, the current FDA-approved dose. The FDA is also reviewing tofacitinib 10 mg and 5 mg twice-daily tablets for treating adults with moderate to severe chronic plaque psoriasis who are candidates for systemic therapy or phototherapy. Tofacitinib is an oral Janus kinase inhibitor.
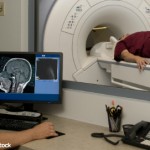
FDA Investigates MRI Safety after Brain Deposits of GBCA Found
The FDA is investigating the risk of brain deposits developing after repeated use of gadolinium-based contrast agents (GBCAs) for magnetic resonance imaging (MRI).3 Recent medical publications have reported that GBCA deposits have remained in patient brains long after the last administration of these agents, particularly in patients who have undergone at least four MRI scans. It is not known whether effects from the gadolinium deposits are harmful or if they can lead to adverse health effects.
The FDA is continuing to study any potential safety risks. No current changes to the product labeling for GBCAs are being recommended at this time.
To prevent the potential accumulation of gadolinium, the FDA is requesting that healthcare professionals limit GBCA use to clinical circumstances in which the additional information provided by the contrast is necessary. The FDA is also requesting that healthcare professionals reassess the necessity of repetitive GBCA MRIs in established treatment protocols.
In published studies, investigators reviewed noncontrast MRIs of patients who had received several GBCA MRIs as part of cancer management, multiple sclerosis management or for other illnesses. The noncontrast MRIs demonstrated findings that suggested gadolinium contrast was being retained in various brain structures. So far there have been no signs or symptoms of adverse health effects and no pathological changes associated with these gadolinium brain deposits. In some of these studies, brain examination at autopsy confirmed gadolinium deposits.
GBCAs include gadofosveset (Ablavar), gadoterate meglumine (Dotarem), gadoxetate disodium (Eovist), gadobutrol (Gadavist), gadopentetate dimeglumine (Magnevist), gadobenate dimeglumine (MultiHance), gadodiamide (Omniscan), gadoversetamide (Optimark) and gadoteridol (ProHance).
FDA Issues Boxed Warning for Hydroxyurea
In regulatory news, the FDA has issued labeling changes—a boxed warning—for Droxia (hydroxyurea). The boxed warning alerts physicians and patients of the possibility of severe myelosuppression with the use of hydroxyurea, with a recommendation to monitor patient blood counts at baseline and throughout treatment.4 The recommendation is to reduce the medication dose and/or stop treatment, as needed. Additionally, patients should be advised to use sun protection while using hydroxyurea and monitor patients for potential malignancies, because the agent is carcinogenic.
Late-Onset Neutropenia Following Rituximab Treatments
A recent study has evaluated the incidence and severity of late-onset neutropenia (LON) following treatment with rituximab (RTX) for patients with rheumatoid arthritis (RA) and other autoimmune diseases (OAIDs).5 Investigators worked with more than 2,500 patients, of whom 1,975 were treated for RA, and all were part of the Autoimmunity and Rituximab (AIR) registry of the French Society of Rheumatology and the Club Rhumatismes et Inflammations. A neutrophil count was requested at inclusion in the registry and at each follow-up visit (three months, six months, then every six months and/or any time treatment changed). Patients were included in the evaluation if they had at least one follow-up.
Neutropenia was defined by an absolute neutrophil count (ANC) of <1,500/mm3. Late-onset RTX-related neutropenia was defined as an ANC of ≤1.5 x 109/L starting at four weeks after completion of RTX therapy until 12 months following the last RTX infusion. LON has mainly been reported following RTX treatment for lymphoma, with sparse data in RA and OAIDs patients.
Follow-up data were collected every six months for up to seven years. Median follow-up for OAIDs patients was 17.4 months (ranging 5.6–29.1; 987 patient-years) and for RA patients it was 24.2 months (ranging 14.7–35.3; 4,179 patient-years). Neutropenia was reported in 85 patients (48 RA and 37 OAIDs). Forty-five patients were excluded due to the presence of neutropenia prior to RTX therapy.
Neutropenia occurred after a median period of 4.5 months (ranging 3–6.5 months), following the last RTX infusion in the RA patients and five months (ranging from 3–6.5 months) in OAIDs patients. One RA patient had neutrophils <500/mm3, seven RA patients had neutrophils between 500 and 1,000/mm3, and 17 RA patients had neutrophils between 1,000 and 1,500/mm3. The OAIDs patients who developed LON were: seven patients with systemic lupus erythematosus, seven patients with vasculitis and one patient with myositis.
Nineteen patients who developed neutropenia after RTX treatment were retreated with RTX. Of those 19, three developed neutropenia again. No patients developed infections or needed growth factor treatment. In the RA patients who developed LON, no baseline risk factors were identified, except age and female gender. LON in RA occurred, but cases were relatively mild. The authors recommend monitoring blood counts following each cycle of RTX.
Michele B. Kaufman, PharmD, CGP, RPh, is a freelance medical writer based in New York City and a pharmacist at New York Presbyterian Lower Manhattan Hospital.
References
- Seattle Genetics Inc. News release: Seattle Genetics initiates clinical trial of adcetris (brentuximab vedotin) in systemic lupus erythematosus, a chronic autoimmune disease. 2015 July 9.
- Pfizer Inc. News Release: Pfizer announces FDA acceptance for review of new drug application for a once-daily formulation of xeljanz (tofacitinib citrate) modified release tablets. 2015 Jul 2.
- U.S. Food and Drug Administration. Drug safety communication: FDA evaluating the risk of brain deposits with repeated used of gadolinium-based contrast agents for magnetic resonance imaging (MRI). 2015 July 27.
- U.S. Food and Drug Administration. Safety Alerts for Human Medical Products: Droxia (hydroxyurea). July 2015.
- Salmon JH, Cacoub P, Combe B, et al. Late-onset neutropenia after treatment with rituximab for rheumatoid arthritis and other autoimmune diseases: Data from the AutoImmunity and Rituximab registry. RMD Open. 2015;1:e000034. doi:10.1136/rmdopen-2014-000034