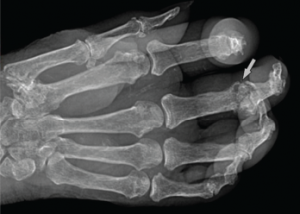
Figure 2: Radiograph of the Right Hand
Note the erosive change (arrow) seen at the head of the proximal phalanx, characterized by its sharp, overhanging edges. Soft tissue swelling can be seen in associated acute inflammatory lesions.
Due to the hematologic abnormalities and the duration of symptoms, colchicine was withheld. She was placed on intravenous solumedrol 40 mg daily, with the intention of tapering the dosage. Initial urate-lowering therapy was deferred until resolution of the acute inflammatory presentation. After 48 hours of IV solumedrol therapy, there was complete resolution of the podagra and polyarticular inflammatory arthritis. However, the bullous lesions remained remarkably tender and continued to expand over the next 24 hours. No new bullous lesions developed, but there was clear increase in size (see Figure 3) of the initial bullae.
Ultrasonography of the small joints of the hands was performed, including the dorsal aspect of the third DIP, where the bullous lesion was located. Ultrasound imaging (see Figure 4) demonstrated a classic cutaneous appearance of “wet sugar clumps” of tophaceous gout just under the surface of the bullous lesion.
The larger of the two lesions was aspirated (see Figure 5), and coarse, granular liquid with the consistency of wet sand was drained. The bullous lesion was rinsed with saline after aspiration and wrapped. Within one day, the patient had significant reduction in pain and tenderness of the aspirated bullous lesion. The same was done for the other lesion with rapid relief, allowing further tapering of corticosteroid therapy and resolution of the progressive inflammatory skin changes. Polarized light microscopy (see Figure 6) demonstrated dense clusters of needle-shaped monosodium urate crystals, with a negatively birefringent appearance.
Discussion
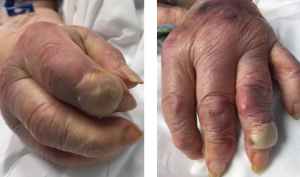
Figures 3A & 3B
Fig. 3A: Enlargement of the creamy, yellow-hued bullae present over the DIP of the second digit of the right hand; and Fig. 3B: DIP of the second digit of the left hand.
Gout, considered the most common form of inflammatory arthritis, affects nearly 4% of the adult population in the U.S.1 Recurrent and exquisitely tender mono- or oligoarticular inflammation is the classic manifestation of the disease, with episodes often resolving within several days, but possibly extending up to weeks in the acute phase.
Examples of gout have been thoroughly documented for centuries and appear to be on the rise in developing countries, as hyperuricemia associated with the metabolic syndrome continues to increase.1,2 Factors contributing to this include dietary changes, with new light being shed on the effects of fructose intake on the risk of developing gout. Surprisingly, fruit juice and other sugar-sweetened beverages appear to carry a higher relative risk of developing incident gout than the consumption of purine-rich meats, classically thought of as the primary culprits of increased dietary urate burden, contributing to hyperuricemia.1 Other factors increasing the risk of incident gout include medications, particularly thiazide and loop diuretics, which contribute to hyperuricemia.1,2
